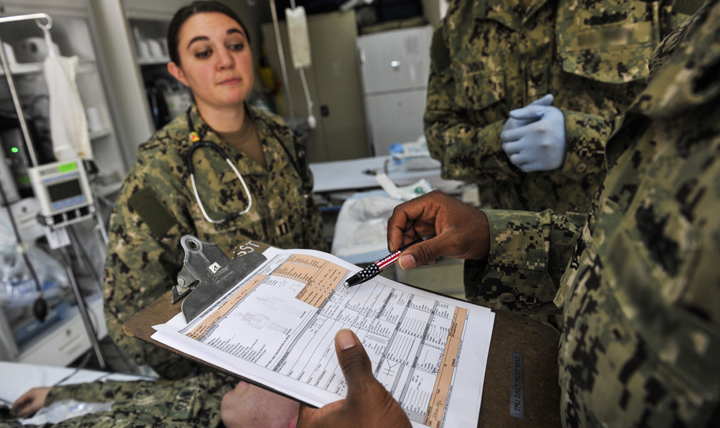
—Doctors gain valuable insight by asking their patients about their family health history. (U.S Navy photo by Mass Communication Specialist 1st Class Eric Dietrich/released)
Health Benefits After EAS
Enrolling for health benefits through the VA is typically a very time-consuming and confusing process. We would recommend that you speak with someone who has already gone through the process, or with a patient service representative (PSR) at the VA before beginning the enrollment process. Remember, you are not alone in this process and there is always some sort of assistance to be provided if you are lost. The paper work is time-consuming, and you will need your DD214 along with additional documents to verify your eligibility.
I had to fill out paperwork with the PSR and give them all my information. I can't remember how long it took for them to approve my enrollment for benefits...almost 6 months if I remember correctly. I then spoke with a counselor and filled out more paperwork to determine if I was qualified to receive disability for PTSD, depression, anxiety, or anything else combat-related. After that I, saw a psychologist to determine if I had any mental disorders; luckily I was good to go. I also took a hearing test, and now I receive roughly $133/month for my 10% hearing disability, and I will get this for the rest of my life. Brian, USMC Veteran
Apply for VA Health Benefits
The very first step in obtaining access to VA Health Benefits is to apply. If your Marine meets the basic eligibility requirements, VA encourages them to apply today by completing and submitting VA Form 10-10EZ, Application for Health Benefits online. Click here to learn more.
You can apply online or at your nearest VA hospital in person and a VA representative will assist you with applying. Applying online is faster and significantly reduces the processing time for enrollment and you will be able to access your health care benefits more quickly. You will need to complete a VA Form 10-10EZ (link above), application for health benefits. Once you complete your information, you may submit the application. You will immediately receive a confirmation message notifying you that your application has been received. Applying in person is typically the same process. Generally, you will receive written notification of your enrollment status in the VA health care system within 5 -7 days. The letter will also give you instructions on how to appeal the decision if you do not agree.
You can also apply over the telephone.
- Call 1-877-222-VETS(8387)
- 8 am to 8 pm Mon-Fri, EST
Complete application over the telephone with a VA representative.Within 3-5 business days you will receive the completed VA Form 10-10EZ, Application for Health Benefits for you to review, sign and return.
Mail the application to:
Health Eligibility Center
2957 Clairmont Road, Suite 200
Atlanta, GA 30329-1647
More information regarding the enrollment process can be found on the website listed above for the VA health benefits enrollment.
Application Process
Click here.Notification of the Status of Your Application
Once your application for enrollment is approved, you will receive a welcome phone call from us to assist you with scheduling your first VA health care appointment and to answer questions you may have about your health care benefits. VA will send you a personalized Veterans Health Benefits Handbook that contains specific information regarding health care benefits you are eligible for, your Enrollment Priority Group assignment, copay status, and other helpful information as a new enrollee.If you are unable to be enrolled or you disagree with the enrollment decision, you may appeal the decision. The handbook will contain information on the appeal process and if you are not able to be enrolled, VA will notify you by letter or the reason why you cannot be enrolled. The letter will contain information and instructions on how to appeal the decision if you do not agree with it.
Basic Eligibility
If you served in the active military service and were separated under any condition other than dishonorable, you may qualify for VA health care benefits. Current and former members of the Reserves or National Guard who were called to active duty by a federal order and completed the full period for which they were called or ordered to active duty may be eligible for VA health benefits as well.
Reserves or National Guard members with active duty for training purposes only do not meet the basic eligibility requirement.
Minimum Duty Requirements
Most Veterans who enlisted after September 7, 1980, or entered active duty after October 16, 1981, must have served 24 continuous months or the full period for which they were called to active duty in order to be eligible. This minimum duty requirement may not apply to Veterans who were discharged for a disability incurred or aggravated in the line of duty, for a hardship or "early out," or those who served prior to September 7, 1980. Since there are a number of other exceptions to the minimum duty requirements, VA encourages all Veterans to apply so that we may determine their enrollment eligibility. For more information, click here.
Health Benefits Explorer (This will be different for everyone)
This helps you estimate and determine your eligibility. It is a series of questions that you need to answer and it will help determine the copays, deductibles, and benefits for healthcare you are to receive. It will then lead you to an enrollment site to get started with the process. Click here to begin
Active Duty
Active Duty Servicemembers who have received their separation and/or retirement orders may apply for enrollment in VA health care system. If eligible, Service members become enrolled upon separation or retirement Click here to apply.
Transitioning from TRICARE to Veteran's Health Benefits
When service members leave active duty, they may be eligible for benefits offered by TRICARE and the VA, depending whether they retire or how they separate from the military. If retiring, a service member is eligible for TRICARE as a military retiree and may be eligible for certain VA benefits. Service members who separate due to a service-connected disease or injury may be eligible for VA health benefits and certain TRICARE benefits.
OEF/OIF/OND combat Veterans can receive cost free medical care for any condition related to their service in the Iraq/Afghanistan theater for five years after the date of their discharge or release. In order to take advantage of these benefits, OEF/OIF/OND Vets need to enroll in VA's health care system.
Returning Service Members
Your service has earned your access to enhanced VA health care benefits. In order to take advantage of these benefits, OEF/OIF/OND Veterans need to enroll in VA's health care system. Click here to learn more.
Enhanced Eligibility For Health Care Benefits
Veterans who served in a theater of combat operations after November 11, 1998 are eligible for an extended period of eligibility for health care for 5 years post discharge.Under the "Combat Veteran" authority, the Department of Veterans Affairs (VA) provides health care services and community living care for any condition possibly related to the Veteran's service in the theater of operations and enrollment in Priority Group 6, unless eligible for enrollment in a higher priority group to: Combat Veterans who were discharged or released from active service on or after January 28, 2003, are eligible to enroll in the VA health care system for 5 years from the date of discharge or release.The 5-year enrollment period begins on the discharge or separation date of the service member from active duty military service, or in the case of multiple call-ups, the most recent discharge date.
Combat Veterans, while not required to disclose their income information, may do so to determine their eligibility for a higher priority status, beneficiary travel benefits, and exemption of copays for care unrelated to their military service.
Who's Eligible?
Veterans, including activated Reservists and members of the National Guard, are eligible if they served on active duty in a theater of combat operations after November 11, 1998, and have been discharged under other than dishonorable conditions.
Are you a combat Veteran and want to find out how this law affects you? Fill out the Returning Service members Calculator:
Click here.
Documentation Used To Determine Service in a Theater Of Combat Operations
- Military service documentation that reflects service in a combat theater, or
- Receipt of combat service medals, and/or
- Receipt of combat tax exemption, imminent danger or hostile fire pay
Health Benefits Under The "Combat Veteran" Authority
- Medical care and medications provided for conditions potentially related to combat service
- Enrollment in Priority Group 6 unless eligible for enrollment in a higher priority group
- Full access to VA's Medical Benefits Package
What Happens After The Enhanced Eligibility Period?
Veterans who enroll with VA under this authority will continue to be enrolled even after their enhanced eligibility period ends. At the end of their enhanced eligibility period, Veterans enrolled in Priority Group 6 may be shifted to a lower priority group depending on their income level, and required to make applicable copays.
Families of Veterans
Under certain circumstances, family members of Veterans are eligible for health benefits. Some of the programs offered include the Civilian Health and Medical Program of the Department of Veterans Affairs (CHAMPVA), Spina Bifida (SB), Children of Women Vietnam Veterans (CWVV), Foreign Medical Program (FMP) and Caregiver. Using these programs may reduce or eliminate your cost for medical supplies, office visits or prescriptions. Click here for more information
Women Veterans
Each VA Medical Center has a Women Veterans Program Manager who is designated to advise and advocate for women Veterans. They can assist Women Veterans with accessing medical services from primary care to specialized care for chronic conditions or reproductive health. Click here to view all that VA health care for women Veterans includes.